Cost-Sharing Reduction cuts: 5 questions answered in response to Trump’s executive order
First, we want to acknowledge how challenging it can be to follow all the developments around Obamacare, healthcare, and insurance. With less than 2 weeks until Open Enrollment for 2018 coverage (which begins on November 1), things can get confusing very fast.
The most recent announcement is the defunding of Cost-Sharing Reduction payments to insurance carriers. You may have quite a few questions about this, and we’re here to make sure you are equipped with the best knowledge possible to make an informed decision about coverage this Open Enrollment.
So what does this mean for you? If you qualify for subsidies, you will still get help paying for coverage — and you may even find a cheaper plan! However, it’s still critical that you shop around and understand the changes being made.
Here are five important questions answered in response to this change:
1. What is a Cost-Sharing Reduction (CSR)?
“Cost-Sharing Reduction” is the industry term used to identify the extra financial help many people get to lower their deductibles and out-of-pocket costs for care and prescription drugs. You must enroll in the Silver plan to get the Cost-Sharing Reduction, and you only qualify if your income is under a certain amount. Specifically, CSR only matters to you if you make less than:

2. Will I still get help paying for coverage?
Yes! Anyone who qualified for financial assistance in the form of the Advanced Premium Tax Credit (also called the “subsidy”) will still receive that. As a refresher, you qualify if you make less than:

If you only qualify for the subsidy that will reduce your monthly premiums and not Cost-Sharing Reduction, you might get a better deal by switching from a Silver plan to a Bronze or Gold plan.
3. Will it cost me more?
If you qualify for subsidies, you shouldn’t see a major difference in cost for the 2018 coverage year – in fact, coverage could be cheaper because of the way that your subsidy is calculated.
If you don’t qualify, you will end up seeing an increase in cost. You should still make sure to shop and see what coverage options are available.
4. What does this mean if I already have Marketplace coverage?
It means you should actively shop around this year because insurance companies have raised prices in different ways. Especially for silver plans, which are popular for those who get substantial subsidies and Cost-Sharing Reductions.
5. Where can I shop and enroll?
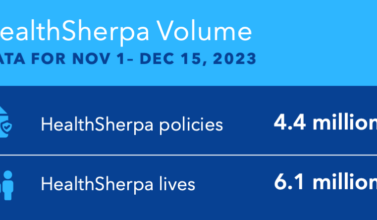
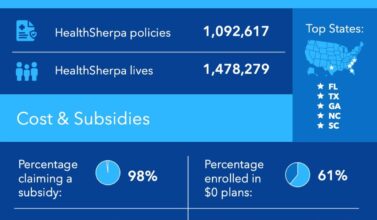
You can shop and enroll on HealthSherpa. HealthSherpa has enrolled over 1M people in Marketplace coverage and has a team of experienced Consumer Advocates available 7 days a week, ready to answer any questions you may have. Call us at (855) 772-2663 or schedule an appointment here.
Don’t forget that the Open Enrollment window is SHORTER this year. It begins on November 1 and you must enroll by December 15 to have coverage for 2018.
We can not stress enough how important it is this year that you shop around for coverage. There has been clear disruption caused by the administration’s actions, and plan prices are changing more than usual. You want to be sure you don’t miss out on getting the most affordable coverage or worse, get stuck paying way too much.
Call us directly at (855) 772-2663 or you can self-enroll on HealthSherpa.com!












This was very helpful and timely, I was very confused when the President made this announcement. Thanks so much for making it simple. As Healthsherpa has done since day one.
You’re welcome! We’re glad it was easy to understand.
Ok…I think you cleared things up. Thanks Kyle 🙂
[…] The widely reported Cost-Sharing Reduction cuts are having a noticeable impact on the plans that people are signing up for: […]